Cardiomyopathy
Cardiomyopathy (ˌkärdēˌōˌmīˈäpəTHē) literally means heart (cardio) muscle (myo) disease (pathy) and is a general term that refers to any condition where the heart muscle (myocardium) function is abnormal. While some people can have a subclinical cardiomyopathy without any obvious symptoms, usually they ultimately end up with heart failure, especially if appropriate treatment is not given. The most common symptoms from heart failure are shortness of breath (dyspnea) and peripheral edema (swelling of the legs) and fatigue. People with cardiomyopathy are often at risk of arrhythmias including atrial fibrillation and more dangerous and life-threatening forms or irregular heart beats such as ventricular tachycardia which can lead to sudden cardiac death.
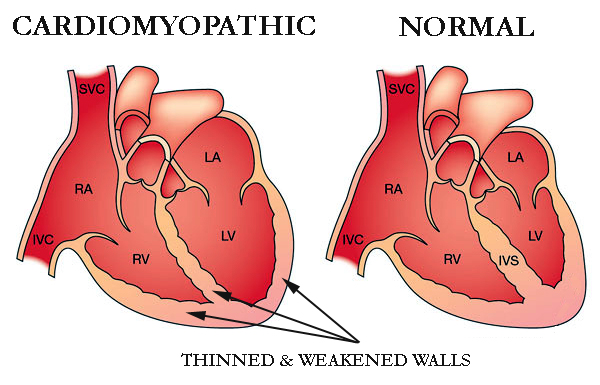
Most cardiomyopathies are due to other conditions that lead to damage of the the myocardium although some cardiomyopathies can be genetic. The most common general form of cardiomyopathy is dilated cardiomyopathy (DCM) where the heart becomes enlarged. It most commonly is caused by prior heart attacks due to coronary artery disease (ischemic cardiomyopathy) or long-standing and uncontrolled hypertension (hypertensive cardiomyopathy). Many other factors can cause or contribute to a cardiomyopathy including certain drugs (including some types of chemotherapy used for cancer such as anthracycline-induced cardiomyopathy) or alcohol (alcoholic cardiomyopathy). Diabetes can also lead to a diabetic cardiomyopathy. Often significant cardiac valve dysfunction is present due to the heart enlarging, such as mitral regurgitation although aortic or mitral regurgitation can lead to dysfunction of the heart muscle and heart failure. In particular, when a patient presents with significant heart failure with severe dysfunction of their heart muscle and significant mitral regurgitation, it often can be difficult to know which came first and whether an intrinsic cardiomyopathy is present or not.
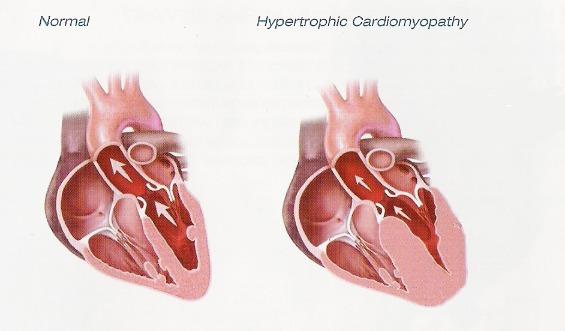
Hypertrophic cardiomyopathy refers to abnormally thickened heart muscle. While a patient with long-standing untreated hypertension might develop significant hypertrophy, the term hypertrophic cardiomyopathy usually refers to a genetically acquired type of cardiomyopathy. It can effect relatively young people who can be at risk of sudden cardiac death (due to life-threatening ventricular arrhythmias) and they sometimes can go on to develop heart failure as well. There are delayed-onset forms of hypertrophic cardiomyopathy that can be seen in the elderly as well.
Cardiomyopathies can be due to infiltration of the heart muscle from metabolic or storage diseases such as due to amyloidosis or hemochromatosis (the latter condition is due to excess iron in the body). Some of these cardiomyopathies can impair or restrict the ability of the heart muscle to adequately relax in between each heart beat leading to heart failure and are classified as a restrictive cardiomyopathy. There are several other, much rarer, forms of cardiomyopathies including ventricular non-compaction (“spongioform cardiomyopathy”); arrhythmogenic right ventricular dysplasia (ARVD); mitochondrial myopathy or cardiomyopathy associated with muscular dystrophy; Takotsubo cardiomyopathy (“stress-induced” cardiomyopathy or “broken-heart syndrome”); and obesity-associated cardiomyopathy. Long-standing overactive thyroid disease (hyperthyroidism) can lead to a cardiomyopathy as can other hormonal imbalances such as acromegaly. Certain vitamin deficiencies can lead to cardiomyopathy as can certain infections including HIV and Chagas Disease. Peri-partum cardiomyopathy can occur in the last trimester of pregnancy, around the time of delivery or soon after and can lead to severe heart failure.
Cardiomyopathy can occur after a fulminant non-specific viral infection leading to acute inflammation of the myocardium known as myocarditis. Cardiomyopathies of unknown etiology are known as idiopathic cardiomyopathy. Treatment of cardiomyopathy would involve treating any underlying causes, but ultimately is usually a matter of routine congestive heart failure treatment with medications. When diagnosed early enough and aggressive medical management in given with frequent regular follow-up, many patients can markedly improve and stabilize in this day and age. When patients do not adequately respond and continue to have significant dysfunction and heart failure, an automated implantable cardiac defibrillator (AICD) might need to be implanted to reduce the risk of sudden cardiac death. Some patients will respond to a special type of pacemaker that “resychronizes” the electrical system of each heart beat to improve the cardiac function. In patients whom continue to have disabling heart failure not adequately responding to the above interventions, a left-ventricular assist device (LVAD) might need to be surgically implanted to support their cardiac function and they might be listed for a heart transplant if they otherwise are an acceptable candidate. Researchers are also working on stem-cell therapy to help improve cardiac function, but this is still considered experimental.
Patients with cardiomyopathy generally should be under the ongoing care of a cardiologist.
Click here for more information on cardiomyopathy.
Updated 01/31/13
Written by and/or reviewed by Mark K. Urman, M.D. and Jeffrey F. Caren, M.D.
PLEASE NOTE: The information above is provided for general informational and educational purposes only and should not be used during any medical emergency. The information provided herein is not intended to be a substitute for medical advice, nor should it be used for the diagnosis or treatment of any medical condition. Accordingly, it should not be relied upon as a substitute for consultation with licensed and qualified health professionals who are familiar with your individual medical needs. Call 911 for all medical emergencies. Links to other sites are provided for information only – they do not constitute endorsements of those other sites. Please see Terms of Use for more information.