Valve Disease
Valvular Heart Disease
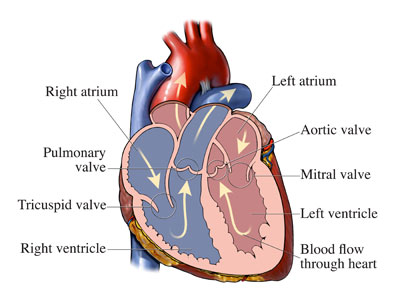
The human heart has four chambers, two on the right side of the heart and two on the left side. The upper chambers accept blood from large veins and are called atria (plural for atrium – just like an entrance hall of a building) and blood is then passed to the lower main pumping chambers, called ventricles. The right atrium receives oxygen-poor blood from the veins of the body, the blood then flows to the right ventricle which pumps blood through the pulmonary (lung) artery to the lungs so that it gets enriched with oxygen. Oxygenated blood then goes through the pulmonary veins into the left atrium and then flows into the left ventricle which pumps blood into the aorta, the biggest and main artery which delivers blood to the body. Click here for more information on how the normal heart works.
Heart valves are tissue flaps that act like doors that open to let blood flow through or out of your heart, and then shut to keep the blood from flowing backward. All of this is highly coordinated with each heart beat. The main function of the valves is to keep blood flowing in one direction through the heart’s chambers and out of the heart to the lungs or body. A heart murmur is a sound that is heard by a physician using a stethoscope that is due to blood flow in the heart. It can be an “innocent” murmur not related to valve disease but it can indicated dysfunction of one or more of the heart valves. An echocardiogram is the most commonly used and useful test to evaluate heart valve function. It is an ultrasound that allows a cardiologist to visualize the heart and all of its valves including whether a valve is not closing adequately or is not opening adequately.
When a valve does not close properly and blood leaks backwards, the backflow is called regurgitation (or sometimes insufficiency). A small amount of regurgitation is usually well tolerated and is not of short-term concern and might not ever worsen or cause a problem. When a significant amount of regurgitation is present, the pumping chamber (ventricle) has to work much harder, pumping a larger amount of blood in a very inefficient manner to try to get enough blood to go forward to meet the demands of the body and can lead to serious problems.
When a valve does not fully open or is restricted in opening, it is called valvular stenosis. This usually is due to the valve tissue thickening or stiffening or fusing together. Mild stenosis is usually well tolerated, not of short-term concern and might not ever worsen to the point of causing a problem. More severe valve stenosis results in a narrowing of the opening that blood normally flows through, making it harder for the blood to be pumped through the valve. The pumping chamber or ventricle ends up working much harder and too much pressure is put on the walls of the heart leading to dysfunction over time.
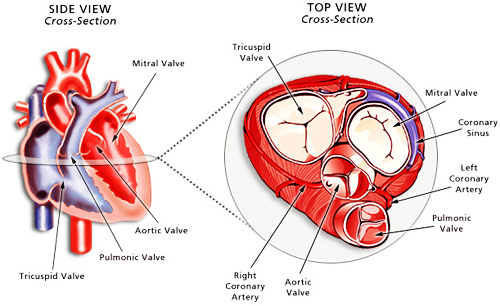
- The aortic valve
- The mitral valve
- The pulmonary or pulmonic valve
- The tricuspid valve.
Heart valve disease occurs when one or more of these valves do not work properly. Click here for more on knowing your valves. The aortic valve allows blood to leave the heart’s main pumping chamber, the left ventricle, and go into the aorta to be delivered to the body. This opening between the left ventricle and aorta is circular and a normal aortic valve has three cusps, each relatively even in size, looking like a “Mercedes-Benz” logo when closed. It opens with each heart beat. The mitral valve has 2 cusps and opens between each heart beat allowing blood to flow from the left atrium into the left ventricle. Similar to the aortic valve, the pulmonary (or pulmonic) valve has 3 cusps and allows blood to go from the right ventricle to the pulmonary artery (delivering blood to the lungs to get oxygen). The tricuspid valve has 3 cusps and allows blood to flow from the right atrium to the right ventricle. Click here for more on understanding heart valve disease.
Valves can degenerate with age and either not fully or properly close leading to regurgitation or they can stiffen and/or thicken with age leading to stenosis. A number of valve structural problems can be present at birth (called congenital valve disease). Valves might not form properly; they may not have enough tissue flaps, they may be the wrong size or shape, or they make lack an opening through which blood can flow properly (called atresia).
Heart valve disease is common, affecting over 5 million individuals in the United States. For some people, the condition will stay largely the same over their lifetime and never need treatment or intervention. For other people, their heart valve problem will worsen over time, eventually requiring medication, medical procedures, or even surgery to repair or replace the defective valve. Usually, more significant valve problems in adults are more serious when on the left side of the heart (aortic or mitral valve) although on occasion severe tricuspid or pulmonic valve problems can be significant. Left untreated, advanced valve disease can cause heart failure, stroke, blood clots, or sudden cardiac death.
Degenerative valve disease, the most common form of valvular heart disease in industrialized nations, is associated with aging and, thus, is an emerging health problem with broad consequences. An estimated 95,000 valve surgery procedures are performed each year in the U.S. and aortic valve disease alone is responsible for more than 25,000 annual deaths. Increasing age is the greatest risk factor for valve disease and an estimated one in eight people age 75 years or older have at least moderate heart valve disease.
Click here to read about and see how the heart works.
DRUG THERAPIES
People with heart valve disease may be prescribed medicines (as required) to treat heart failure, lower blood pressure or prevent irregular heartbeats, known as arrhythmias. Since several valve diseases or defects make people susceptible to blood clots, blood thinning drugs are sometimes recommended. These medications are required in people who have undergone surgery and now have one or more man-made or “mechanical” valves. For many years, patients with various heart valve problems were instructed to take antibiotic prophylaxis prior to dental work and certain medical procedures in order to reduce the risk of endocarditis (an infection of the heart valves). These recommendations have changed, and far fewer patients now need to take these prophylactic antibiotics. The only patients who still require them are those with artificial heart valves, patients with complex congenital heart disease, and patients who have previously experienced endocarditis. If you have a heart valve abnormality but are not sure if you still need to take antibiotics prior to dental visits and other medical procedures, please check with your physician.
NATURAL HISTORY
Heart valve disease is usually a lifelong condition. Over time, the problem may worsen and require more than medications can offer. In these cases, valve repair or replacement may be indicated. Patients with heart valve disease are routinely evaluated and followed by cardiologists. Once you have undergone such a surgical procedure for valve disease, you may still need certain medications, and will require regular checkups for the rest of your life.
Technical considerations
Valve repair or replacement may be recommended for advanced valve disease or in people with less advanced disease but at high risk of lasting damage to their heart without surgical intervention. Whether heart valve repair or replacement is selected may depend on a number of factors, such as severity of the valve disease and your age and general health.
Mitral Regurgitation
Based on better outcomes, mitral valve repair is especially recommended over mitral valve replacement for the majority of patients with longstanding severe mitral regurgitation. Referral of patients with severe mitral regurgitation to surgical centers experienced in mitral valve repair is recommended as mitral regurgitation requiring surgical intervention should be surgically repaired if technically feasible. Newer non-surgical techniques to repair mitral regurgitation are being developed but are still considered experimental.Click here for more information on mitral regurgitation.
Aortic Stenosis and Aortic Regurgitation
Click here for more information on aortic stenosis.
Click here for more information on aortic regurgitation.
Tissue or mechanical valve?
Patients who require valve surgery but in whom repair is not feasible may be offered a metal (mechanical) valve or a tissue (bioprosthetic) valve (from a pig or human cadaver). Tissue valves offer the great advantage of not requiring the use of blood thinners after implantation, but are not as long lasting as mechanical valves. This means that if a tissue valve is implanted in a young individual, a repeat valve replacement surgery is highly likely during that patient’s lifetime. The decision to implant a tissue valve versus a mechanical valve therefore needs to include patient age and patient lifestyle issues (e.g. desire to play competitive sports, in which case the tendency to bleed easily due to the presence of blood thinners would not be ideal). The guidelines recommend a patient age of 65 years as the threshold for implantation of a tissue as opposed to a mechanical valve in the aortic and mitral positions. The guidelines also make an allowance for patient preference to recommend a bioprosthesis in a patient under 65 years of age. In addition, improvements in durability of newer bioprosthetic tissue valves appear to be leading them to last longer, thus younger patients are opting for tissue valves more and more.
Non-surgical techniques
Although not widely available, there are some newer surgeries that utilize less invasive means to access the valves for surgical repair or replacement. These procedures use smaller incisions, cause less pain, and speed recovery time. Some cardiologists and cardiac surgeons are exploring these new procedures that are still largely experimental.
Valve disease and pregnancy
Usually, mild-to-moderate heart valve disease during pregnancy can be successfully managed through pregnancy, labor, and delivery with conservative measures such as medications and bed rest. Severe heart valve disease, however, can make pregnancy or labor and delivery much riskier than normal. Ideally, management of women with valve disease should begin before conception. A careful examination and assessment of heart function is needed to determine whether an individual woman will be able to tolerate the stresses on the heart during pregnancy, labor, and delivery. Women with severe valve disease should talk to their doctor about the option of valve repair or replacement before getting pregnant. These surgeries can be performed during pregnancy, but they increase the danger to both mother and fetus.
Click here for more information on heart valve disease from the American College of Cardiology (Cardiosource)

Click here for more information on heart valves and treatment options from Edwards Lifesciences (YourHeartValve.com)
Updated 11/06/15
Written by and/or reviewed by Mark K. Urman, M.D. and Jeffrey F. Caren, M.D.
PLEASE NOTE: The information above is provided for general informational and educational purposes only and should not be used during any medical emergency. The information provided herein is not intended to be a substitute for medical advice, nor should it be used for the diagnosis or treatment of any medical condition. Accordingly, it should not be relied upon as a substitute for consultation with licensed and qualified health professionals who are familiar with your individual medical needs. Call 911 for all medical emergencies. Links to other sites are provided for information only – they do not constitute endorsements of those other sites. Please see Terms of Use for more information.