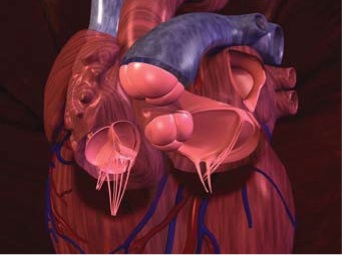
Mitral Valve
These leaflets are supported by thin string-like cords similar to those that support parachutes and serve to prevent the valve from bulging in the opposite direction toward the atrium when the ventricle contracts. When the atrium contracts, the mitral valve opens to allow the blood to flow toward the ventricle. When the ventricle contracts, the mitral valve closes to prevent the blood from flowing back toward the atrium. When the mitral valve does not fully close and leaks (i.e. blood flows backwards) it is called mitral regurgitation. A trivial or mild amount of mitral regurgitation is considered within normal physiological limits. Concern is raised when the mitral regurgitation becomes moderate to severe.
In summary, mitral regurgitation is a condition in which the valve between the heart’s two left chambers doesn’t close all the way, and allows some blood to flow backward. If it becomes significant, mitral regurgitation makes the heart work harder and can lead to heart failure.
Mitral valve prolapse
Mitral valve prolapse occurs when one or both flaps “prolapse,” that is to say, they bulge toward the atrium when the ventricle contracts. This can happen if the leaflets are very large or if the cords supporting them are too long. When prolapse occurs, the valve does not close tightly and blood can leak backward through the mitral valve. The doctor often can hear the mitral valve prolapse when he or she listens to the heart. This prolapse can cause a sound like a click. If the blood flows back (backwards) through the valve, the doctor may hear a murmur. The doctor may order a test called echocardiography to take images of the heart in order to confirm the diagnosis and see if the mitral valve leaks.
Symptoms of mitral valve prolapse
Most patients with mitral valve prolapse have no symptoms. But some patients do have symptoms associated with mitral valve prolapse. These can include chest pain, palpitations or feeling that the heart is beating fast and skipping beats, having dizzy spells or light-headedness, shortness of breath and a feeling of panic or anxiety.
Treatment of mitral valve prolapse
Unless there is a murmur associated with a valve that leaks or symptoms that are bothersome, no treatment is needed. The patient most likely will not have problems and will not need treatment. However, patients who have valves that leak will need to have periodic follow-up exams and/or echocardiograms as sometimes the leak can worsen or cause the heart muscle to weaken. No medications have been proven to change the course of mitral valve prolapse or regurgitation although if high blood pressure is present, it definitely should be treated. The latest and most recent recommendations are that most patients with mitral valve prolapse or mitral regurgitation do not routinely need to take antibiotics before undergoing dental procedures or cleaning to prevent the valve from becoming infected (endocarditis). Unfortunately, while routine prophylactic endocarditis prophylaxis has not been proven to be effective, patients with significant mitral valve prolapse or regurgitation are at increased risk of endocarditis.
Surgical options for Mitral Regurgitation:
When mitral regurgitation becomes severe, whether due to mitral valve prolapse or due to other causes, there is a significant risk of developing a weakening of the left ventricle which can lead to congestive heart failure. The heart has to work much harder when a significant amount of the blood it is pumping is going backwards. Patients with significant mitral regurgitation also are at higher risk of developing arrhythmias such as atrial fibrillation. Ideally, the mitral regurgitation should be surgically corrected before the heart starts to show signs of damage. This is because often the damage is permanent and the heart will not fully recover even after successful surgical repair. Sometimes this means that surgery might be indicated even if the patient has no symptoms because of signs of deterioration that a cardiologist observes, usually on an echocardiogram.
Valve surgery is recommended in patients with chronic severe mitral regurgitation if they have any symptoms, atrial fibrillation or pulmonary hypertension (increased blood pressures in the lungs). Surgery is also recommended for patients without symptoms if their left ventricular (LV) pumping function is impaired (ejection fractions < 60%) or their LV is significantly enlarged.
Cardiac surgeons with adequate experience can often repair the mitral valve rather than having to replace it. A successful mitral valve repair usually leads to better outcomes than a mitral valve replacement. Less invasive methods to repair mitral valves that leak are being developed including robotic options such as are being used by our cardiac surgical colleagues at the Cedars-Sinai Heart Institute. Current research is being done on non-surgical methods to repair mitral valves including non-surgical means. One method that involves a clip (MitraClip by e-Valve) was performed at the Cedars-Sinai Heart Institute on more patients than anywhere else in the world in a recent large trial with very promising initial results. Those with significant mitral valve prolapse or mitral regurgitation, should see their cardiologist regularly and discuss what their best options might be.
Click here for a printer friendly version of this article.
For more information on heart valve disease, click here.
Written by and/or reviewed by Mark K. Urman, M.D. and Jeffrey F. Caren, M.D.
Updated 03/19/13
PLEASE NOTE: The information above is provided for general informational and educational purposes only and should not be used during any medical emergency. The information provided herein is not intended to be a substitute for medical advice, nor should it be used for the diagnosis or treatment of any medical condition. Accordingly, it should not be relied upon as a substitute for consultation with licensed and qualified health professionals who are familiar with your individual medical needs. Call 911 for all medical emergencies. Links to other sites are provided for information only – they do not constitute endorsements of those other sites. Please see Terms of Use for more information.